A Strategy for Health Plans: Activating Social Determinants of Health
The impact of Social Determinants of Health (SDoH) on member outcomes has loomed large with health plans for over a decade.
Social Determinants of Health
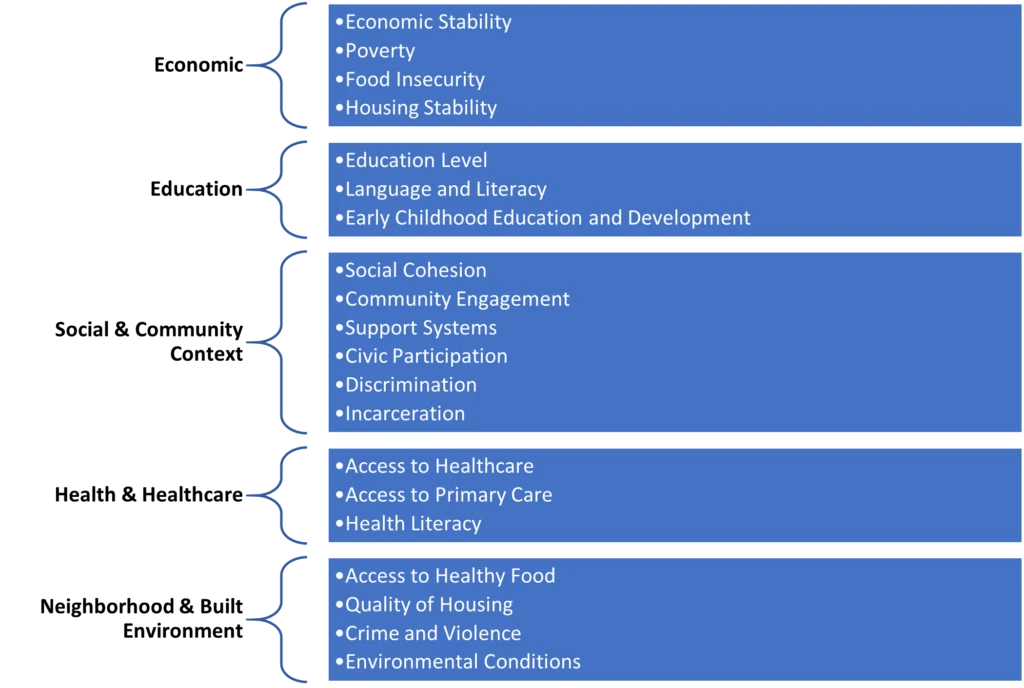
Source: www.cdc.gov
Health Plans have realized that by mitigating the negative impacts of SDoH, they can achieve substantial benefits. These benefits will certainly improve access and outcomes for members. These changes will also lower overall costs. Subsequently, health plans have implemented several successful large-scale community programs to address SDoH for their members. They have also implemented the inclusion of SDoH as part of benefit design and care management workflows. Even with the success of these SDoH program initiatives, members will continue to fall through the cracks. A robust infrastructure needs to be put into place to identify targeted members, ensure accountability in the delivery of social services, measure key indicators from member data, and extrapolate insights.
The Microsoft Cloud for Healthcare, and its trusted partners, provided a prosperous solution —an integrated, data-centric platform grounded in capabilities that empower better experiences, better insight, and better care. In the context of SDoH, the Microsoft Cloud for Healthcare enables Health Plans to activate SDoH, which essentially transforms data into action. This is an ongoing challenge, but this process has improved clinical, social, and behavioral outcomes for members.
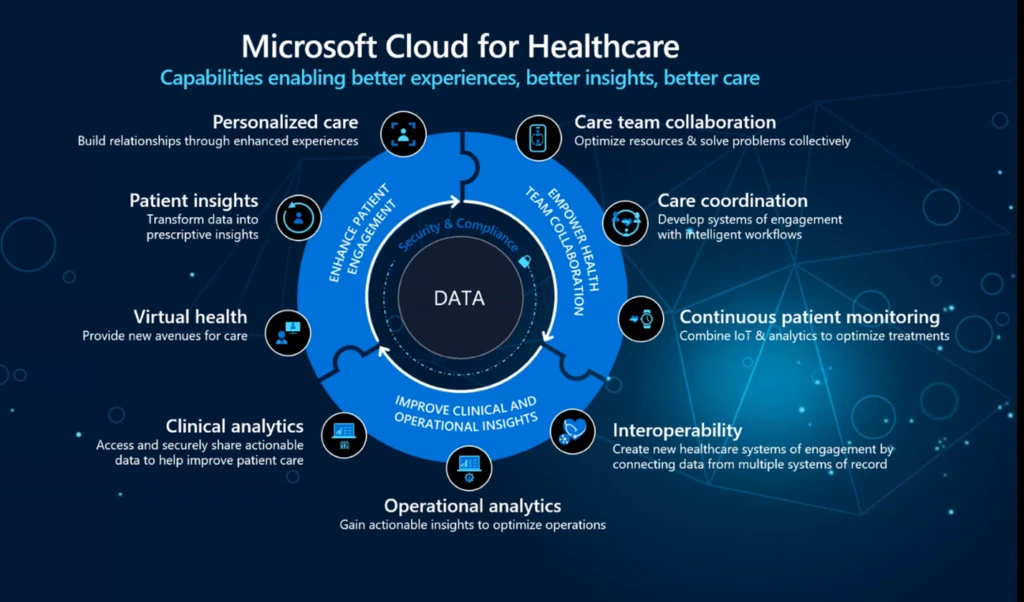
SDoH Activation
SDoH Activation is dependent on four key capabilities, which ensure personalized member experiences, holistic care, and the ability to track and measure the impact of SDoH interventions.
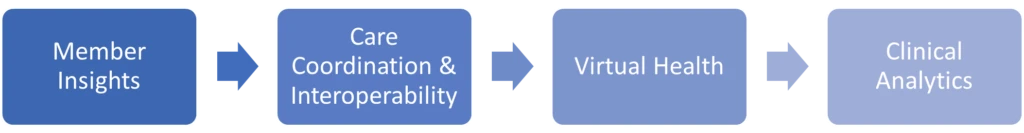
Member Insights
- Microsoft’s trusted partner, Jvion, created a specific solution to SDoH. Jvion’s SDoH solution identifies socioeconomic barriers that are influencing members’ health risks. This is a significant shift from a primarily claims-based [predictive] model to a model that includes social and behavioral indicators. This type of model provides a much clearer representation of the “whole” member. The new model is better equipped to predict the total costs of future care and targeted, individualized interventions, which will aid in aligning community benefits more effectively. The platform also gives insights into potential investments healthcare organizations can make in community benefit programs to address gaps in care.
- Microsoft’s 365 platform provides an integrated view of members’ preferences, interactions, and history across clinical and customer service needs.
Care Coordination & Interoperability
- Coordination of services is dependent on multiple capabilities. API FHIR enables connectivity with community partnerships and social service agencies, while Azure AI/BI can prioritize social services aligned to local market supply and member needs. Dynamics 365 enables the coordination and tracking of bidirectional referrals across the network.
Virtual Health
- Microsoft Teams provides a more accessible, connected, data-driven, and seamless member experience. It is an accessible, easy-to-use platform that allows care managers to outreach and engage at-risk, vulnerable members to address social isolation and loneliness, mental/behavioral health counseling and treatment, and deliver effective care management.
Clinical Analytics
- Gaps and inconsistencies in data can make it difficult to understand the impact of SDoH interventions on health outcomes. With Power BI, Health Plans can track SDoH trends across member populations and measure the impact of interventions. Reports can be generated that include screenings, searches, referral outcomes, and additional performance indicators.
The Microsoft Cloud for Healthcare provides an infrastructure to support end-to-end care coordination, which further enables Health Plans to extend their existing SDoH outreach by activating effective capabilities that address their most vulnerable populations. These actions include screening, identifying, prioritizing, connecting, and optimizing support for their members with specific SDoH needs. Ultimately, addressing SDoH is about leveraging people and technology. This model reflects a shift from traditional care models to ones that achieve “whole-person” care, which aligns with reducing costs and improving member outcomes.